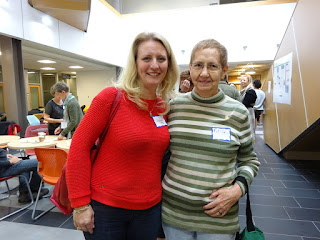Significant updates: 12 Feb. 2022 (See #3 below:In memoriam:Dr. David Ferguson)
December's blog is about eight pathologists, hematopathologists and hematologists, I've had the pleasure to work with over a more than 50-year transfusion career. I cannot do them justice so will offer a series of brief tidbits that symbolize how I see them. Some are what folks call 'real characters,' some not, but they all have strength of character and I'll never forget any of them.1. John Bowman (Winnipeg, Manitoba)
I've blogged on Jack before when he died in 2005:
Dr. Jack Bowman (In Memoriam)
Many tidbits to show why I respected him.
The rest are from my career in Edmonton, Alberta, Canada.
2. Lynn K. Boshkov (Edmonton)
Lynn is such an unassuming person. Loved her tenure at the UAH transfusion service. She was the Medical Director when this case happened
So respected her when she disclosed and explained what had happened to the patient's family whose loved one had died and supported the staff member involved. Lynn eventually moved to Portland's Oregon Health and Science University.
3. David Ferguson (Edmonton)
As UAH Medical Director David helped me a lot as the clinical instructor to the UAH transfusion service. He eventually moved to BC and later retired. Two tidbits:
The Med Director gave oral exams to all med lab technologist doing their clinical rotation at UAH and I was present to decrease any stress. Once David asked a student which lectin acted like anti-A1. Her reply was Delicious biflorus (not Dolichos biflorus) at which point he started laughing uncontrollably. Poor kid, I tried to salvage the moment, though I had a huge grin on my face.
Second tidbit is David's reaction to feedback we got on a paper submitted to AABB's Transfusion.
Letendre PL, Williams MA, Ferguson DJ. Comparison of a commercial hexadimethrine bromide method and low-ionic-strength solution for antibody detection with special reference to anti-K. Transfusion 1987 Mar-Apr;27(2):138-41.
AABB reviewers thought we needed to change title to add 'with special reference to anti-K'. We did, of course, but I'll never forget David's venting as only he could do. In retrospect I wish all could see him as I did.
In Memoriam - David Ferguson: Recently learned of that David died on January 3, 2022.He'll be sadly missed by all of Canada's transfusion medicine community.
4. Ed Uthman (MEDLAB-L)
When I created the mailing list MEDLAB-L in 1994, Ed was one of the first to subscribe. He soon became a rockstar and motivated many to love the list and join. He contributed many posts and made the list a success.
5. Neil Blumberg (MEDLAB-L)
Neil also joined MEDLAB-L early on and was so generous with answering questions completely and in detail. The wealth of knowledge he has is incredible and that he's so willing to take time to share it with others.Wow!
6. Ira Shulman (MEDLAB-L)
Ira gave talk at Edmonton conference and I got to know him. Came to my University of Alberta Med Lab Sci office to catch up on e-mail. I erred in ordering wine that was sweet at a local restaurant (horrors!) and especially funny as I prefer very dry wine. We went to the local IMAX theatre as he wasn't into a river valley walk.
Great guy. Loved California Blood Bank Society (CBBS e-network forum) but it ended.
Once he asked me to present at AABB conference with him, but without financial support as a consultant I couldn't, especially given the US-Canada exchange rate. At ISBT World Congress in Vancouver I enjoyed his OMG comment on all the backup files I had for my Powerpoint presentation.
6. Heather Hume (Ottawa, CBS Head Office)
I worked on contract for CBS under Heather's supervision, along with colleague and friend Kathy Chambers, when Heather was executive medical director, and had the vision that CBS should do more transfusion education. Heather is special.
Together, with input from Dr. Lucinda Whitman, we created a Transfusion Medicine website [screen shot of old site] that has since transmogrified to Professional Education.
At Vancouver at ISBT 2002 Congress when, as a panel member, I noted I'd stayed at University of Alberta Med Lab Sci for 22 years but managed only 9 months at CBS Edmonton as 'Assman,' Heather quipped,~ to 'Pat always wants to end with a laugh.' I'm sure she was thinking much worse, but the classy lady gave me the benefit of the doubt.
7. Gwen Clarke (Edmonton)
I taught Gwen when she was in Med Lab Sci and got to know her better after she became a hematopathologist. In 2006 Gwen and Morris Blajchman edited Clinical Guide to Transfusion, the first to be published online and in print. Believe it or not, I was a co-author (minuscule role) of one of its chapters:
8. Susan Nahirniak
I count Susan as one of my Med Lab Sci 'kids'. Despite all my kooky blogs and tweets, Susan never fails to greet me with a warm smile, as here at MLS 2018 reunion. I so appreciate that she forgives me my sins for old time's sake. During our talk her phone kept vibrating because her daughter wanted to be picked up, but Susan kindly ignored the phone.
In summary, I hope you enjoyed these glimpses into encounters I've had with a variety of transfusion physicians over the decades. All are very different, unique, and superb representatives of their profession.
TWEETS
Replies I received on Twitter when I posted this blog. Both have given me permission to post their tweets.
#1 By @shroon7, 1 Jan. 2019
I adored Dr. Boshkov and was @UBB [University of Alberta Blood Bank] as an LAII when she left. Dr. Clarke is also wonderful and I’m glad I still get to talk to her occasionally when she’s on call. RBB’s [Royal Alexandra blood bank] loss was CBS’s gain.Dr. N [Nahirniak] is another fave; more than a few times I’ve been very glad it was her on call. #2 By @shroon7, 1 Jan. 2019
She [Lynn Boshkov] was just so wonderfully “chill” in bone marrows. She had the best ability to keep patients distracted and at-ease during the whole procedure.
#3 By @shroon7, 1 Jan. 2019
To sum up: Considering THREE fabulous hemepaths I’ve had the good fortune to work with are three of your top choices after your long career, I’d consider myself very blessed.
#1 By @DoctorCanBob, 1 Jan. 2019
Lynn was trained in McMaster and was also a superb "clotter".
#2 By @DoctorCanBob, 1 Jan. 2019
Lynn is still doing primarily clotting in Portland at OSMU.
Also see entire thread of these tweets.
FOR FUN
Could choose many songs for this blog but decided on 'Those Were The Days' by Mary Hopkin. Her 1968 version, produced by Paul McCartney, became a number one hit in UK.
As always, feedback is appreciated. See Comments below.
4. Ed Uthman (MEDLAB-L)
When I created the mailing list MEDLAB-L in 1994, Ed was one of the first to subscribe. He soon became a rockstar and motivated many to love the list and join. He contributed many posts and made the list a success.
- NOTE: Both Ed Uthman and Neil Blumberg gave me permission to post their MEDLAB-L messages.
- Ed's reply to me asking if the list was an anachronism (Beauty!)
5. Neil Blumberg (MEDLAB-L)
Neil also joined MEDLAB-L early on and was so generous with answering questions completely and in detail. The wealth of knowledge he has is incredible and that he's so willing to take time to share it with others.Wow!
- Typical Neil reply to a question asked by a list subscriber
- Reply on low lab morale that shows Neil's character
6. Ira Shulman (MEDLAB-L)
Ira gave talk at Edmonton conference and I got to know him. Came to my University of Alberta Med Lab Sci office to catch up on e-mail. I erred in ordering wine that was sweet at a local restaurant (horrors!) and especially funny as I prefer very dry wine. We went to the local IMAX theatre as he wasn't into a river valley walk.
Great guy. Loved California Blood Bank Society (CBBS e-network forum) but it ended.
Once he asked me to present at AABB conference with him, but without financial support as a consultant I couldn't, especially given the US-Canada exchange rate. At ISBT World Congress in Vancouver I enjoyed his OMG comment on all the backup files I had for my Powerpoint presentation.
6. Heather Hume (Ottawa, CBS Head Office)
I worked on contract for CBS under Heather's supervision, along with colleague and friend Kathy Chambers, when Heather was executive medical director, and had the vision that CBS should do more transfusion education. Heather is special.
Together, with input from Dr. Lucinda Whitman, we created a Transfusion Medicine website [screen shot of old site] that has since transmogrified to Professional Education.
At Vancouver at ISBT 2002 Congress when, as a panel member, I noted I'd stayed at University of Alberta Med Lab Sci for 22 years but managed only 9 months at CBS Edmonton as 'Assman,' Heather quipped,~ to 'Pat always wants to end with a laugh.' I'm sure she was thinking much worse, but the classy lady gave me the benefit of the doubt.
7. Gwen Clarke (Edmonton)
I taught Gwen when she was in Med Lab Sci and got to know her better after she became a hematopathologist. In 2006 Gwen and Morris Blajchman edited Clinical Guide to Transfusion, the first to be published online and in print. Believe it or not, I was a co-author (minuscule role) of one of its chapters:
2006 Chamber K, Letendre P, Whitman L. Blood Components. In: Clinical Guide to Transfusion, Clarke G, Blajchman M, eds. Ottawa: Canadian Blood Services, 2006.Every technologist who works with Gwen respects her. She's a oner. I hope CBS knows how lucky they are to have her on staff.
8. Susan Nahirniak
I count Susan as one of my Med Lab Sci 'kids'. Despite all my kooky blogs and tweets, Susan never fails to greet me with a warm smile, as here at MLS 2018 reunion. I so appreciate that she forgives me my sins for old time's sake. During our talk her phone kept vibrating because her daughter wanted to be picked up, but Susan kindly ignored the phone.
In summary, I hope you enjoyed these glimpses into encounters I've had with a variety of transfusion physicians over the decades. All are very different, unique, and superb representatives of their profession.
TWEETS
Replies I received on Twitter when I posted this blog. Both have given me permission to post their tweets.
#1 By @shroon7, 1 Jan. 2019
I adored Dr. Boshkov and was @UBB [University of Alberta Blood Bank] as an LAII when she left. Dr. Clarke is also wonderful and I’m glad I still get to talk to her occasionally when she’s on call. RBB’s [Royal Alexandra blood bank] loss was CBS’s gain.Dr. N [Nahirniak] is another fave; more than a few times I’ve been very glad it was her on call. #2 By @shroon7, 1 Jan. 2019
She [Lynn Boshkov] was just so wonderfully “chill” in bone marrows. She had the best ability to keep patients distracted and at-ease during the whole procedure.
#3 By @shroon7, 1 Jan. 2019
To sum up: Considering THREE fabulous hemepaths I’ve had the good fortune to work with are three of your top choices after your long career, I’d consider myself very blessed.
#1 By @DoctorCanBob, 1 Jan. 2019
Lynn was trained in McMaster and was also a superb "clotter".
#2 By @DoctorCanBob, 1 Jan. 2019
Lynn is still doing primarily clotting in Portland at OSMU.
Also see entire thread of these tweets.
FOR FUN
Could choose many songs for this blog but decided on 'Those Were The Days' by Mary Hopkin. Her 1968 version, produced by Paul McCartney, became a number one hit in UK.
As always, feedback is appreciated. See Comments below.